Testicular heat stress: is one of the reason for male infertility? When there is raised temperature, inner testicular temperature is also raised leading to Testicular heat stress. This causes sperms of inferior quality.
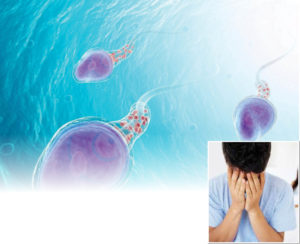 The testicles or testis are core organs of the male reproductive system. Covered by a sac called scrotum, the two egg shaped testicles hang between the legs – they make sperms and male hormone testosterone. The other important intra – testicular structures are vas deferens, seminiferous tubules, epididymis and the tunica covering layers. Germ cells in the seminiferous tubules help in making the sperms. Leydig cells located between the seminiferous tubules release testosterone, the male hormone that helps germ cells make sperm.
The testicles or testis are core organs of the male reproductive system. Covered by a sac called scrotum, the two egg shaped testicles hang between the legs – they make sperms and male hormone testosterone. The other important intra – testicular structures are vas deferens, seminiferous tubules, epididymis and the tunica covering layers. Germ cells in the seminiferous tubules help in making the sperms. Leydig cells located between the seminiferous tubules release testosterone, the male hormone that helps germ cells make sperm.
Infertility
Barrenness, lack of fertility, subfertility, infecundity or lack of fertility and lack of fruitfulness are all expressions to indicate the inability to conceive. Infertility as a term applies to both genders and is defined as: a disease of the reproductive system defined by the failure to achieve a clinical pregnancy after 12 months or more of regular unprotected sexual intercourse (WHO-ICMART glossary)”, this definition is available at the national portal of GOI. While female infertility is spoken of widely, TOI, dated, 14.1.19 report has stated 50% of infertility cases is male infertility. Important aspects reflecting male infertility are loss of libido or decreased desire to have sex, erectile dysfunction, difficulty in ejaculation, low sperm count and sperm problems, and decreased volume of ejaculate. Male infertility cases may have repeat respiratory infections, inability to smell and decreased facial hair. Male infertility cases have less than 1.50 crore sperms per ml of spermathecal fluid. Normal sperm count is 1.50 crores to 20.00 crores sperms per ml of spermathecal fluid.
Mayo clinic, USA communication states about infertility cases: 1/3rd are male infertility, 1/3rd are female infertility and in another 1/3rd cases, the causes are unknown or there are health issues in both males and females. There are many causes of male infertility: structural and functional problems of male reproductory system including premature ejaculation, physical problems (metabolic issues, obesity etc), chemical and environmental factors like smoking, alcohol, side effects of certain medications, pollutants and cancer treatments.
There are many causes of male infertility: structural and functional problems of male reproductory system including premature ejaculation, physical problems (metabolic issues, obesity etc), chemical and environmental factors like smoking, alcohol, side effects of certain medications, pollutants and cancer treatments.
Testicular temperature and male infertility
There is a hypothermic testis in male humans – it means there is reduced temperature in the testicles. The testicular temperature is normally 2 to 4 degree Celsius less than core body temperature. Sperm formation is temperature dependent. There is proper sperm formation only when testis temperature is slightly lower than rest of body. When there is raised scrotal temperature, inner testicular temperature is also raised leading to what is called as genital heat stress. This causes sperms of inferior quality. Heat stress damages sperm cells. Such sperms have damaged DNA, poor fertilizing capacity and can even die prematurely. Scrotum structure, tissues and functioning is such that it helps maintain lower temperature in the testicles.
Human sperm production in the testicles requires 72 days, and only 12% of the total sperms produced have fertilization potential. Rest of the sperms are defective or die prematurely. Sperm formation is best when there is an optimal temperature range in the testes. Increase of even 1 degree centigrade scrotal temperature results in 14% drop in sperm formation inside the testes. Scrotal temperature minimum of 2 degrees below core body temperature is best for sperm formation. Normal body temperature is 37 degree centigrade and sperm formation is ideal with scrotal temperature at 34 degree centigrade or Celsius. (Celsius or centigrade refer to same units). Generally speaking, normal testis temperature is 35 degrees Celsius.
What causes raised scrotal temperature?
- Scrotal position: hanging testis has better and easy heat dissipation. The unclothed and upright body has least scrotal temperature. When walking, scrotal temperature is lower due to good heat dissipation and air circulation. In one study, seated male paraplegics on wheel chairs with unmoving thighs had higher deep scrotal temperature and less motile sperms compared to able bodied men who sat freely. Testicular temperature increases when movement is minimized such as in prolonged sitting where scrotum is resting between the thighs closely. ‘Sitting disease’ certainly compounds the problem of male infertility. Seated position increases scrotal temperature
- Heated seats: prolonged sitting on heated surfaces such as heated car seat or heated floor further adds to the increased scrotal temperature due to sitting
- Layers of clothing and bedding that traps heat: Clothing can increase temperature by upto 2 degree centigrade. Similarly, tight underwear may contribute to raised genital temperature through less air circulation
- Long term sustained hot baths and saunas also have a negative effect on semen quality
- The use of laptops and mobiles on the lap close to genital area causes dip in all sperm parameters
- Long hours of cycling with tight clothing and being seated on the saddle seat elevates scrotal temperature
- Other factors: obesity where excess scrotal and other types of abdominal fat raises scrotal temperature, radiant heat due to occupational reasons (eg., welders), and pathological abnormalities in scrotal region, including repeat fevers causes abnormal sperm parameters.
Fitness is a government supported trend in India, today. Being fit implies healthy habits, exercise and walking, and nourishing oneself with good food. A fit body and good lifestyle almost always supports good fertility in males and females. Small things such as appropriate change in seat, dress, bedding, clothing and other lifestyle factors will ensure absence of deleterious effect on the male reproductive system. Good health comes from a fitness attitude. A fit attitude of males, means a robust and well-maintained male reproductive system that avoids heat stress on testicles.

Sunil S Chiplunkar
M Pharm (Pharmacology) MBA (Marketing) PGDHRM
VP – Training (Marketing), Juggat Pharma:
Pharma division of Jagdale Ind. Pvt. Ltd.,
Bangalore – 560078 Ph.: 9379077788
email : sunilchiplunkar@gmail.com
www.pharmaceuticalshealthcare.blogspot.in